Editorial Note:
This article is an expanded and revised edition of a previously commissioned feature. It has been updated to clarify a common misconception: high uric acid is not only a “gout issue”. Even without classic gout flares, persistently elevated uric acid is associated with kidney stones, kidney strain, and cardiometabolic risk factors that often cluster together (high blood pressure, insulin resistance, and high cholesterol).
Key takeaways (quick read):
- Uric acid can be high with no symptoms, until complications (stones, gout attacks) appear.
- It is closely tied to metabolic health (weight, insulin resistance, blood pressure, triglycerides).
- Diet changes help most, but “purines” is not the whole story — hydration and sugary drinks/alcohol often matter just as much.
Quick action today: if you have a history of gout, kidney stones, high blood pressure, fatty liver, or diabetes/prediabetes, consider asking for a uric acid test at your next check-up and review your results in context of overall metabolic health.
When most people hear about high uric acid, they immediately think of gout—a condition infamous for causing sudden, severe pain in the joints, often the big toe. However, the reality is that elevated uric acid, or hyperuricaemia, is a much broader health concern. It is a silent, often overlooked risk factor that can quietly undermine your health, even if you never experience a single gout attack.
What is Uric Acid?
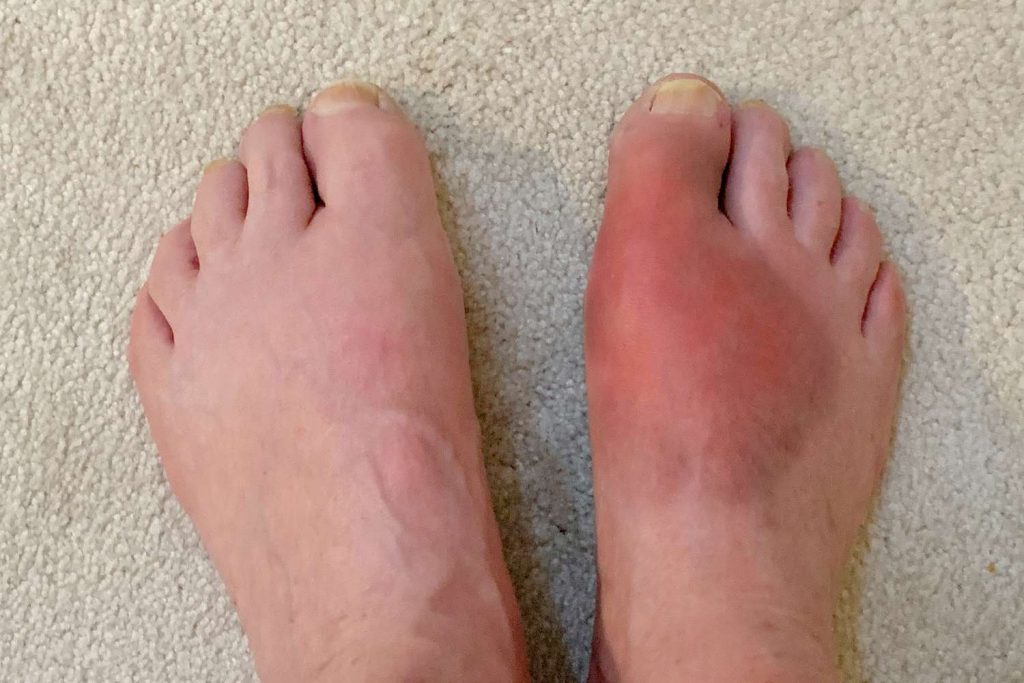
Uric acid is a waste product formed when the body breaks down purines, which are natural substances found in your body’s cells and in many foods, especially red meat, organ meats, seafood, and certain alcoholic beverages. Normally, uric acid dissolves in the blood, passes through the kidneys, and is excreted in urine. However, if your body produces too much uric acid or your kidneys do not eliminate enough, uric acid can accumulate in the blood.
There are two main reasons for elevated uric acid: increased production and decreased excretion. Increased production can result from a diet high in purines, rapid cell turnover (as seen in some cancers), or certain genetic factors. Decreased excretion is often due to kidney dysfunction, dehydration, or the use of certain medications such as diuretics.
Obesity, metabolic syndrome, and insulin resistance are also strongly linked to higher uric acid levels. In fact, hyperuricaemia is frequently seen in people with high blood pressure, high cholesterol, and type 2 diabetes. These conditions often cluster together, compounding the risk of cardiovascular disease.
The Role of Dietary Habits
Diet plays a crucial role in determining uric acid levels. Whilst animal-based purines (from red meat, organ meats, and seafood) tend to have a stronger effect, plant-based foods also contribute to overall purine intake. In many cultures, certain plant-based foods such as pulses and legumes (like chickpeas, lentils, and beans) are dietary staples and primary sources of protein and nutrients. Whilst these foods are generally healthy and nutritious, they also contain moderate amounts of purines. For most people, moderate consumption does not pose a significant risk, but those with a predisposition to hyperuricaemia or already elevated uric acid levels should be mindful of their overall purine intake.
Beyond Gout: The Broader Health Risks
Whilst gout is the most dramatic manifestation of high uric acid, research over the past decade has revealed that hyperuricaemia is associated with a range of other health problems.
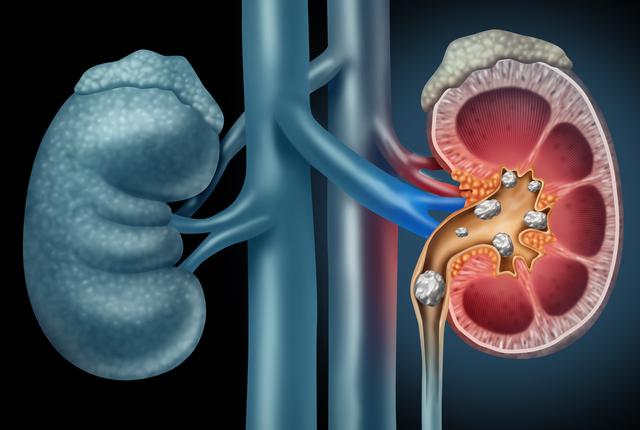
High uric acid can lead to kidney stones, chronic kidney disease, and is now recognised as an independent risk factor for hypertension, coronary artery disease, heart failure, and stroke. Studies suggest that for every 1 mg/dL increase in uric acid, the risk of ischaemic stroke rises by 10 per cent. It is also linked to metabolic syndrome and diabetes, and may play a role in fatty liver disease and cognitive decline.
Who is at Risk?
Anyone can develop high uric acid, but certain groups are more vulnerable. These include people with a family history of gout or kidney stones, those who are overweight or obese, individuals with high blood pressure or diabetes, and those who consume diets rich in purines or alcohol. Men are generally at higher risk than women, though the risk for women increases after menopause.
Several lifestyle and dietary factors can raise uric acid levels, including a diet high in red meat, organ meats, shellfish, oily fish, and alcohol (especially beer), as well as sugary drinks. A diet consistently high in purine-containing plant-based foods, whilst generally healthy, can contribute to uric acid issues in susceptible individuals. Dehydration, obesity, chronic kidney disease, certain medications, and genetics also play a role.
Diagnosing High Uric Acid—Now Easier Than Ever
Traditionally, diagnosing high uric acid required a visit to a clinic or laboratory for blood tests, with results taking hours or even days. However, advances in medical technology have made it possible to monitor uric acid levels quickly and conveniently at home. This empowers individuals to monitor their health more closely, make informed decisions, and manage conditions like gout, diabetes, and metabolic syndrome more effectively—without the need for frequent clinic visits.
Managing and Lowering Uric Acid
Lifestyle changes can significantly reduce uric acid levels and lower the risk of complications. Limit red meat, organ meats, shellfish, and alcohol. Moderate the intake of purine-containing plant-based foods, and ensure a balanced diet with plenty of vegetables, fruits, whole grains, and low-fat dairy. Stay hydrated, maintain a healthy weight, and exercise regularly. Some studies suggest that drinking black coffee in moderation may help lower uric acid. In severe cases, medication may be necessary.
The Importance of Regular Monitoring
Because high uric acid often causes no symptoms until complications arise, regular monitoring is essential, especially for those with risk factors. High uric acid is a silent but significant health risk that extends far beyond gout. It is closely linked to kidney disease, heart disease, stroke, and metabolic syndrome. By understanding the causes, recognising the risks, and making informed lifestyle choices, you can protect yourself from the hidden dangers of hyperuricaemia and maintain better long-term health.
A Practical Uric Acid Plan: What to Track, What to Change, When to Escalate
“Lower your uric acid” advice often gets reduced to “avoid red meat”. That is partly true for some people, but it is incomplete. Uric acid is influenced by kidney excretion, hydration status, alcohol, fructose/sugary drinks, body weight, and insulin resistance. Use the plan below to make changes that actually move the needle.
1) Start with the context: high uric acid is a signal, not a diagnosis
- Some people have high uric acid for years with no gout attacks.
- Risk rises when high uric acid overlaps with kidney disease, stones, hypertension, or metabolic syndrome.
- Numbers matter, but so does your overall risk profile and symptom history.
2) A 2-week reset (focused on the biggest drivers)
- Hydration: aim for pale-yellow urine most of the day (unless you have fluid restrictions).
- Cut liquid sugar: reduce sweetened drinks/juice and frequent sweet coffees/teas (fructose can raise uric acid).
- Alcohol check: reduce frequency and quantity, especially beer; avoid “binge” patterns.
- Protein quality: keep portions moderate; rotate in fish, eggs, tofu/tempeh and legumes rather than relying on red/processed meat daily.
- Fibre baseline: build meals around vegetables and whole grains where tolerated, to support metabolic health.
3) “Purines” explained without the fear-mongering
Purines matter most for some people with gout, but the response varies by individual. Animal-based purine sources (organ meats, certain seafood) tend to be more strongly linked with gout flares. Plant foods that contain purines (legumes, some vegetables) are generally nutritious — many people tolerate them well, and they may support weight and metabolic health, which can indirectly help uric acid.
4) What to ask your clinician (to avoid guessing)
- Should we repeat uric acid and also check kidney function (eGFR/creatinine) and urine results?
- Do my medications (e.g., diuretics) affect uric acid?
- Given my history (stones/gout/CKD), should I consider medication to lower uric acid?
- What target should I aim for, and how often should I monitor?
5) When to seek urgent care
- Sudden, severe joint pain with swelling and redness (possible acute gout flare)
- Severe flank/back pain, nausea/vomiting, or blood in urine (possible kidney stone)
- Fever or feeling very unwell alongside urinary symptoms (possible infection)
Medical note: This article is for general education and is not a substitute for medical advice. If you have kidney disease, recurrent stones, are pregnant, or take long-term medications, consult a qualified clinician before making major dietary changes or starting supplements/medication for uric acid control.
Editorial update: 22 February 2026 — expanded with a 2-week reset plan, a clearer “purines” explainer, and a clinician-question checklist.
Note: This piece was written as a commissioned feature and has appeared in other health and lifestyle platforms.