Editorial Note:
This article is an expanded and revised edition of a previously commissioned feature. It has been updated to clarify a key point: high cholesterol is not always lifestyle-driven. For some people, it is inherited — most commonly as familial hypercholesterolaemia (FH) — which can push LDL (“bad”) cholesterol dangerously high from young adulthood (or earlier), even in people who eat well and exercise.
Key takeaways (quick read):
- FH is common and underdiagnosed — and can cause early heart attacks and strokes if untreated.
- Family history is a major clue: early heart disease or very high cholesterol in relatives should trigger screening.
- Treatment works: early detection + medication (often statins) can reduce risk dramatically and protect whole families via cascade screening.
Quick action today: ask relatives about any early heart attack/stroke and whether anyone has been told they have very high LDL. Bring that information to your next health check.
When most people think of high cholesterol, they picture unhealthy diets, lack of exercise, or ageing. However, for many, high cholesterol is not just a result of lifestyle—it can be inherited. In Singapore, a new national programme is shining a spotlight on genetic cholesterol conditions, offering hope for early detection and better management.
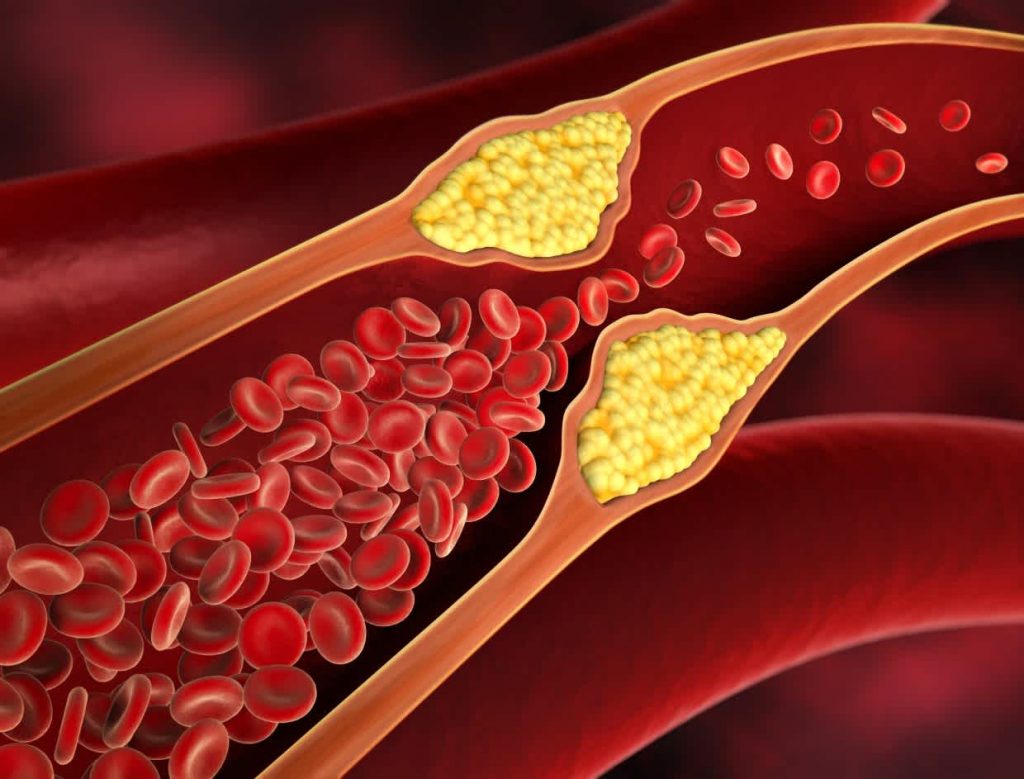
One of the most common inherited cholesterol disorders is familial hypercholesterolaemia (FH). This genetic condition causes dangerously high levels of low-density lipoprotein (LDL), often called "bad" cholesterol, from a young age. Unlike lifestyle-related high cholesterol, FH is caused by mutations in genes responsible for removing LDL from the blood. As a result, cholesterol builds up in the arteries, significantly increasing the risk of heart disease and stroke—even in people who are otherwise healthy and active.
It's estimated that FH affects about 1 in 250 people worldwide. In Singapore, this means that potentially over 20,000 people could be living with FH, but many remain undiagnosed. According to the Ministry of Health, cardiovascular disease is the leading cause of death in Singapore, accounting for nearly 1 in 3 deaths. Early heart attacks and strokes are often linked to undiagnosed or untreated high cholesterol, including genetic causes.
Why Early Detection Matters
People with FH can develop cholesterol deposits in their skin, tendons, or around the eyes, but often there are no obvious symptoms until a serious event occurs. Early detection is crucial because:
- Heart disease can strike early: Individuals with untreated FH may develop heart disease in their 30s or 40s, or even earlier. In Singapore, heart disease is the second leading cause of death, and premature heart attacks are not uncommon.
- Family risk: FH is inherited in an autosomal dominant pattern, meaning each child of an affected parent has a 50% chance of inheriting the condition. This makes family screening essential.
- Effective treatment is available: With early diagnosis, lifestyle changes and cholesterol-lowering medications (such as statins) can dramatically reduce the risk of heart disease. Studies show that with proper treatment, people with FH can have a normal life expectancy.
Singapore's New National Programme
Recognising the importance of early detection, Singapore has launched a new national programme to screen for genetic cholesterol conditions like FH. Under this initiative, Singaporeans can undergo genetic testing to identify if they carry mutations linked to FH and other inherited lipid disorders.
Key features of the programme include:
- Accessible testing: The programme makes genetic testing for FH available to more Singaporeans, especially those with a family history of high cholesterol or early heart disease. The National University Heart Centre, Singapore (NUHCS) and National Heart Centre Singapore (NHCS) are amongst the institutions leading this effort.
- Family-based approach: If one person is diagnosed, their close relatives are encouraged to get tested as well, helping to identify and protect entire families. This "cascade screening" approach is proven to be effective in finding undiagnosed cases.
- Personalised care: Those found to have FH will receive tailored advice and treatment plans, including medication, dietary guidance, and regular monitoring. This is crucial, as studies in Singapore have shown that many with high cholesterol are not on optimal treatment.
- Public awareness: The initiative also aims to educate the public about the genetic risks of high cholesterol and the importance of family health history. According to a 2022 survey, only about 1 in 5 Singaporeans are aware that high cholesterol can be inherited.
The Local Impact
- High cholesterol is common: According to the 2020 National Population Health Survey, about one in three adults in Singapore has high cholesterol (hyperlipidaemia).
- Under-diagnosis is a problem: It is estimated that up to 90% of people with FH in Singapore remain undiagnosed, putting them at risk of early heart disease.
- Treatment gaps: Even amongst those diagnosed, many are not receiving adequate treatment or follow-up, highlighting the need for better awareness and care pathways.
What You Can Do
If you have a family history of high cholesterol or early heart disease, speak to your doctor about genetic testing for FH. Even if you feel healthy, knowing your genetic risk can help you take proactive steps to protect your heart.
Tips for managing cholesterol—genetic or otherwise:
- Eat a balanced diet low in saturated fats and trans fats
- Exercise regularly—aim for at least 150 minutes of moderate activity per week
- Avoid smoking and limit alcohol intake
- Get your cholesterol checked regularly, especially if you have a family history
- Take prescribed medications as directed
A Step Forward for Heart Health
High cholesterol is not always a matter of lifestyle—sometimes, it's in your genes. Singapore's new national programme for genetic cholesterol screening is a major step forward, offering families the chance to detect and manage inherited risks before they lead to serious health problems. By embracing early detection and personalised care, Singapore is helping its people take control of their heart health for generations to come.
If you or your family members have a history of high cholesterol or early heart disease, don't wait—speak to your doctor today about genetic screening. Early action could save your life.
FH vs “Regular” High Cholesterol: A Clear Next-Step Guide
If you have high cholesterol, the most important question is not whether you “failed” at diet and exercise. It is whether your pattern suggests familial hypercholesterolaemia (FH) — because if it does, lifestyle changes alone are rarely enough, and early treatment can be life-saving.
1) The FH “clue list” (bring this to your doctor)
- LDL cholesterol has been very high from a young age
- Close relatives with early heart attack (often before 55 in men, before 60 in women) or early stroke
- Multiple family members with “high cholesterol” across generations
- Cholesterol deposits (in some people): tendon xanthomas or a pale ring around the cornea (not always present)
2) What to ask for at a health check
If you have a strong family history or very high LDL, ask about:
- A fasting lipid panel (total cholesterol, LDL, HDL, triglycerides)
- Other risk markers your clinician may consider (e.g., blood pressure, HbA1c/diabetes screening)
- Whether your history fits criteria for FH assessment and if genetic testing is appropriate
3) Why cascade screening is the “family lifesaver”
FH is commonly inherited in an autosomal dominant pattern — meaning each first-degree relative (parent, sibling, child) may have a meaningful chance of being affected. When one person is diagnosed, screening close relatives can identify others early, before symptoms appear. This is one of the most effective prevention strategies in cardiovascular medicine.
4) Practical lifestyle changes that still matter (even with FH)
- Prioritise fibre (vegetables, legumes, oats, whole grains) and reduce ultra-processed foods
- Choose more fish, soy, nuts, and unsaturated fats; reduce frequent deep-fried meals
- Move regularly (aim for at least 150 minutes/week moderate activity)
- Avoid smoking; manage sleep and stress
But if you have FH, lifestyle is the foundation — it is often not the full treatment.
Frequently asked questions
If I’m slim and active, can I still have FH?
Yes. FH is genetic. Fitness helps overall risk, but it does not “switch off” inherited LDL patterns.
Does taking medication mean I can ignore diet?
No. Medication lowers LDL effectively, but a heart-protective lifestyle supports blood pressure, inflammation, weight, and long-term vascular health.
Medical note: This article is for general education and is not a substitute for medical advice. If you have chest pain, breathlessness, fainting, or stroke-like symptoms, seek urgent medical care. For personalised cholesterol targets and treatment, consult a qualified clinician.
Editorial update: 22 February 2026 — expanded with an FH clue list, a “what to ask for” checklist, and clearer guidance on cascade family screening.
Note: This piece was written as a commissioned feature and has appeared in other health and lifestyle platforms.