Editorial Note:
This article is an expanded and revised edition of a previously commissioned feature. It has been updated to make one key idea clearer: type 2 diabetes and fatty liver disease often travel together, largely because they share the same underlying drivers (especially insulin resistance). If you manage one without paying attention to the other, you may miss an important opportunity to reduce long-term risk.
Key takeaways (quick read):
- Fatty liver can be silent for years — normal day-to-day “energy levels” do not rule it out.
- Diabetes increases the risk of more severe fatty liver (NASH/fibrosis), and fatty liver increases future diabetes risk.
- Small, sustained weight loss (often 5–10%) plus movement can improve both glucose control and liver fat.
Quick action today: if you have type 2 diabetes, prediabetes, central weight gain, or high triglycerides, ask your clinician whether you should be screened for fatty liver and how often your liver markers should be reviewed.
Diabetes and fatty liver disease are two of the most common chronic health conditions in Singapore, and their prevalence is rising rapidly. Whilst they may seem like separate issues, research has shown a strong and complex link between the two. Understanding this connection is crucial for early intervention, better management, and the prevention of serious complications.
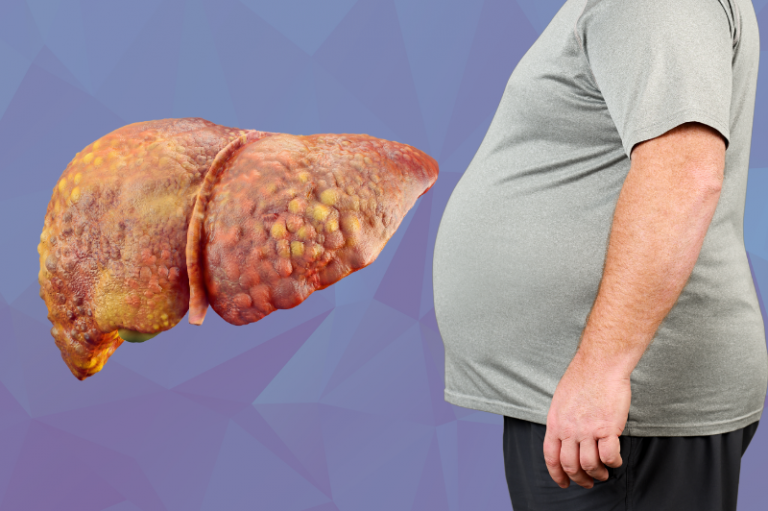
What is Fatty Liver Disease?
Fatty liver disease, also known as hepatic steatosis, occurs when excess fat accumulates in the liver. The most common form is non-alcoholic fatty liver disease (NAFLD), which is not caused by excessive alcohol consumption. NAFLD can range from simple fat accumulation (steatosis) to more severe inflammation and liver damage, known as non-alcoholic steatohepatitis (NASH). If left unchecked, NASH can progress to liver fibrosis, cirrhosis, and even liver cancer.
The Diabetes–Fatty Liver Link
The relationship between diabetes—particularly type 2 diabetes (T2D)—and fatty liver disease is bidirectional and mutually reinforcing:
Insulin Resistance
Insulin resistance is a hallmark of both T2D and NAFLD. When the body's cells become less responsive to insulin, blood sugar levels rise, and the liver starts to store more fat. This process not only increases the risk of developing diabetes but also accelerates the progression of fatty liver disease.
Shared Risk Factors
Obesity, sedentary lifestyle, unhealthy diets, and genetic predisposition are common risk factors for both conditions. In Singapore, the rising rates of obesity and diabetes are mirrored by an increase in NAFLD cases, even amongst younger adults. The local diet, which can be high in refined carbohydrates, sugar, and saturated fats, further contributes to this trend.
Worsening Outcomes
People with diabetes are more likely to develop severe forms of fatty liver disease, including NASH and cirrhosis. Conversely, those with NAFLD are at higher risk of developing T2D. The presence of both conditions significantly increases the risk of cardiovascular disease, kidney problems, and liver-related complications.
Why This Matters in Singapore
Singapore has one of the highest diabetes rates in the world. As of 2024, more than 400,000 people in Singapore are living with diabetes, and this number is projected to reach 1 million by 2050 if current trends continue. The prevalence of diabetes amongst adults aged 20–79 is about 11.6%—one of the highest in the developed world IDF Diabetes Atlas.
Fatty liver disease is also a growing concern. Local studies estimate that up to 40% of people with type 2 diabetes in Singapore also have NAFLD. In the general population, NAFLD affects about 1 in 3 adults, and the numbers are rising, especially amongst younger Singaporeans due to increasing rates of obesity and sedentary lifestyles. Many people are unaware they have fatty liver disease, as it often presents no symptoms until advanced stages.
This "double burden" is particularly concerning because both conditions can progress silently, only becoming apparent when serious complications arise. For example, diabetes is a leading cause of kidney failure and blindness in Singapore, whilst advanced fatty liver disease can result in liver failure or cancer.
Signs, Symptoms, and Screening
Both diabetes and fatty liver disease can be silent in their early stages. Some warning signs to watch for include:
- Persistent fatigue
- Unexplained weight gain, especially around the abdomen
- Elevated liver enzymes on blood tests
- Abdominal discomfort or fullness
However, many people experience no symptoms at all. This is why regular screening is so important, especially for those with risk factors such as obesity, family history, or existing diabetes.
Screening for NAFLD is recommended for people with T2D, obesity, or metabolic syndrome. This can be done through blood tests (checking liver enzymes), ultrasound scans, or more advanced imaging if needed. Early detection allows for timely intervention, which can halt or even reverse liver damage.
Prevention and Management
The good news is that both diabetes and fatty liver disease are largely preventable and manageable with lifestyle changes and, when necessary, medication:

Healthy Diet
Focus on whole grains, lean proteins, healthy fats, and plenty of fruits and vegetables. Limit sugary drinks, processed foods, and foods high in saturated fat. In Singapore, this means being mindful of popular local dishes that may be high in sugar or oil, such as sweetened drinks, kaya toast, or fried foods.
Regular Exercise
Aim for at least 150 minutes of moderate-intensity activity per week. Activities like brisk walking, cycling, or swimming are excellent choices and can be easily incorporated into daily routines.
Weight Management
Even modest weight loss (5–10% of body weight) can significantly improve liver health and blood sugar control. For many, this can be achieved through small, sustainable changes in diet and activity.
Regular Monitoring
People with diabetes should have their liver function checked regularly, and those with fatty liver should monitor their blood glucose levels. Early intervention is key to preventing progression.
Medical Support
In some cases, medication may be needed to manage blood sugar, cholesterol, or liver inflammation. Newer diabetes medications, such as GLP-1 receptor agonists and SGLT2 inhibitors, have shown promise in improving both blood sugar and liver health.
The Role of Innovative Monitoring
Continuous glucose monitoring (CGM) and regular health screenings can help detect changes early, allowing for timely intervention. Devices like CGMs empower individuals to track their glucose trends and make informed lifestyle choices, which can benefit both diabetes and liver health. The CGM can provide real-time feedback, helping users understand how their meals, activity, and habits affect their glucose levels—crucial for those at risk of both conditions.
Singapore's "War on Diabetes" campaign has raised awareness, but more can be done at the individual level. If you have risk factors—such as being overweight, having a family history, or belonging to a higher-risk ethnic group (Malays and Indians in Singapore have consistently higher rates)—speak to your doctor about screening for both diabetes and fatty liver disease.
Employers, schools, and community groups can also play a role by promoting healthy eating, physical activity, and regular health checks. Early detection and intervention not only improve individual health but also reduce the burden on Singapore's healthcare system.
Take Action Today
The link between diabetes and fatty liver disease is strong and often overlooked. In Singapore, where both conditions are on the rise, understanding this connection and taking proactive steps—through healthy living, regular screening, and innovative monitoring—can help prevent serious complications and improve quality of life.
If you are at risk or already living with diabetes, speak to your healthcare provider about screening for fatty liver disease and how you can take charge of your health today. Early action can make all the difference.
What to Do Next (If You Have Diabetes, Prediabetes, or “Borderline” Fatty Liver)
Many people only discover fatty liver when a routine blood test shows raised liver enzymes — and even then, liver enzymes can be normal. The more useful approach is to treat fatty liver as a metabolic risk flag: it’s a sign to tighten up glucose, weight, blood pressure, lipids, sleep and alcohol patterns, and to ask whether further risk assessment is needed.
1) The three screening questions worth asking
- Given my profile, should we do an ultrasound (or other imaging) to assess liver fat?
- Do I need fibrosis risk stratification (blood-based scores and/or elastography), rather than “watch and wait”?
- How often should we recheck HbA1c, triglycerides, ALT/AST and weight/waist measures?
2) A 30-day plan that targets both glucose and liver fat
- Build meals around protein + vegetables first: this often blunts glucose spikes and reduces hunger later.
- Carb quality and portions: choose less-refined carbs; if you use rice/noodles/bread daily, try a smaller portion and add fibre.
- Move after meals: 10–15 minutes of walking after lunch/dinner can improve post-meal glucose control.
- Strength twice weekly: muscle improves insulin sensitivity (bodyweight training counts).
- Sleep as a glucose tool: aim for a consistent schedule; sleep debt worsens insulin resistance.
3) Alcohol: the nuance most articles skip
Fatty liver is often labelled “non-alcoholic”, but alcohol can still worsen liver inflammation and add hidden calories. If you drink, discuss with your clinician what “low risk” looks like for you — especially if you already have diabetes, raised triglycerides, or known liver fat.
4) Medication questions (for people with T2D)
Newer diabetes medicines (including GLP-1 receptor agonists and SGLT2 inhibitors) may support weight loss and improve metabolic markers, which can benefit liver health for some people. This is not a DIY decision — it is worth a targeted conversation about overall cardiometabolic risk, not just glucose numbers.
Frequently asked questions
Can I have fatty liver if I’m not overweight?
Yes. It is more common with excess weight, but genetics, visceral fat distribution, diet and insulin resistance can still play a role.
Do normal liver enzymes mean my liver is fine?
Not necessarily. Liver enzymes can be normal even when liver fat (and sometimes fibrosis risk) is present. Risk assessment is about the whole picture.
Medical note: This article is for general education and is not a substitute for medical advice. Seek medical assessment if you have persistent right-sided abdominal pain, yellowing of the eyes/skin, dark urine, unexplained swelling, or if you have diabetes and are unsure what screening you need.
Editorial update: 22 February 2026 — expanded with a “next steps” screening script, a 30-day dual-target plan, and FAQs on normal liver enzymes and lean fatty liver.
Note: This piece was written as a commissioned feature and has appeared in other health and lifestyle platforms.