Editorial Note:
This article is an expanded and revised edition of a previously commissioned feature. It has been updated to add an important clarity point: brittle or slow-growing toenails are not a “cholesterol symptom” by themselves — they can be a clue of reduced circulation (such as peripheral arterial disease), which is a wider cardiovascular red flag. The update below explains what else to look for, what to ask your doctor for, and how to act without panic.
Key takeaways (quick read):
- Toenails are a clue, not a diagnosis: many conditions can change nail health.
- Circulation signs matter: leg pain when walking, cold feet, slow-healing sores and reduced pulses should be checked.
- Best next step is objective testing: lipid profile + blood pressure + glucose; consider ABI if PAD symptoms are present.
Quick action today: if you have nail changes plus walking leg pain or slow-healing foot sores, book a medical review and ask if a simple circulation check (e.g., pulses/ABI) is appropriate.
High cholesterol is often referred to as the "silent killer" for a reason—it rarely causes obvious symptoms, yet it can quietly and progressively increase your risk of life-threatening conditions such as heart attacks and strokes. Whilst most people associate cholesterol problems with heart health, recent findings highlight a surprising warning sign that could be spotted in your toenails, offering a potentially life-saving clue to your cardiovascular well-being.
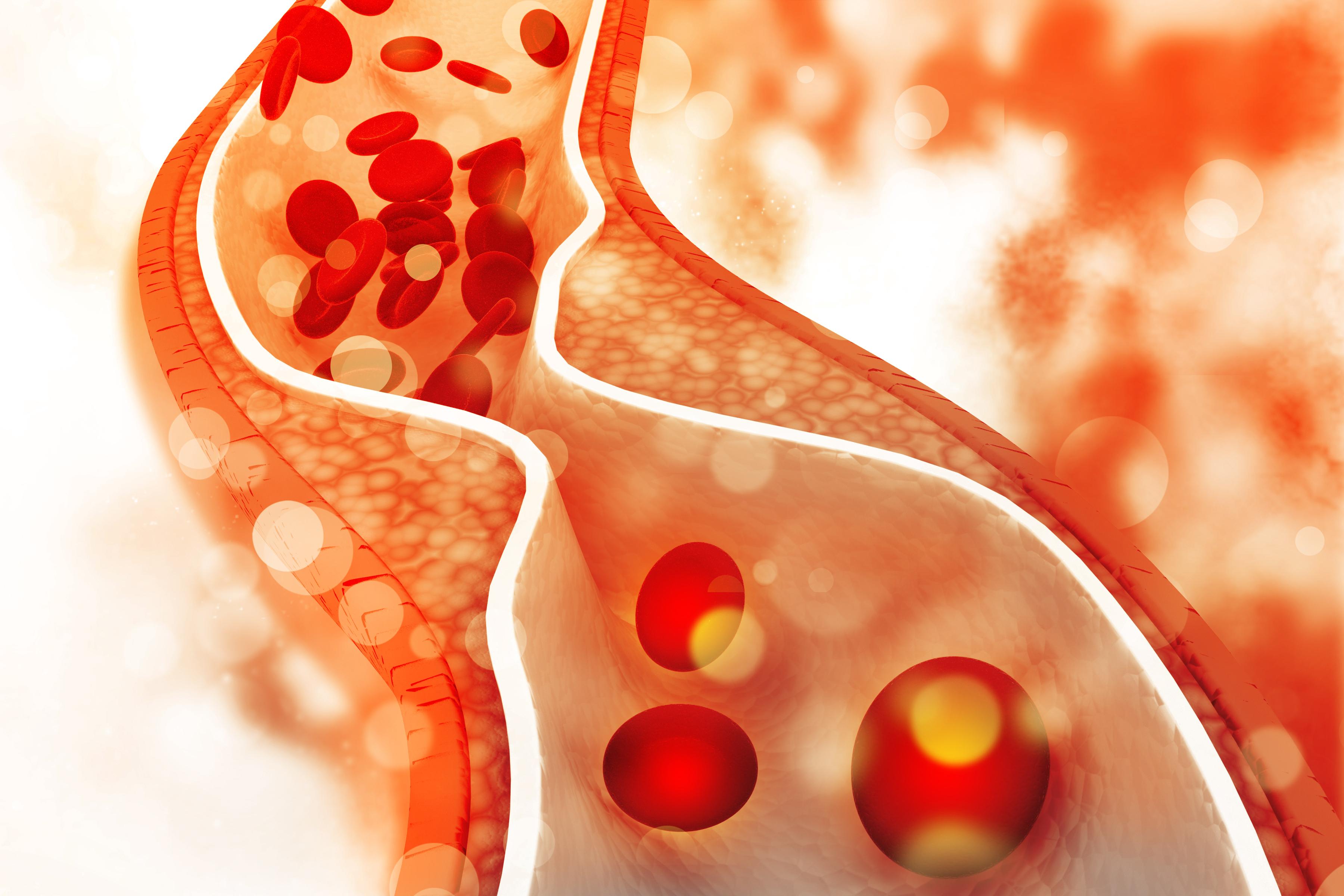
Understanding Cholesterol and Its Risks
Cholesterol is a waxy, fat-like substance found in every cell of your body. It is essential for building healthy cells, producing hormones, and aiding digestion. However, when cholesterol levels become too high—particularly low-density lipoprotein (LDL), often called "bad" cholesterol—it can accumulate in the walls of your arteries. This build-up, known as atherosclerosis, narrows the arteries and restricts blood flow, significantly increasing the risk of heart disease and stroke.
Globally, cardiovascular diseases are the leading cause of death, responsible for an estimated 18 million deaths each year, according to the World Health Organisation. In Singapore, the situation is equally concerning. According to the Singapore Heart Foundation, cardiovascular disease accounted for 32% of all deaths in 2022—meaning that nearly 1 in 3 deaths in Singapore was due to heart disease or stroke. The Ministry of Health (MOH) also reports that about 1 in 3 Singaporeans has a cholesterol level higher than recommended, putting a significant portion of the population at risk.
The Silent Nature of High Cholesterol
One of the most dangerous aspects of high cholesterol is its lack of symptoms. The NHS states: "High cholesterol does not usually cause symptoms. You can only find out if you have it from a blood test." Many people are unaware of their condition until they experience a serious event, such as a heart attack, or have their cholesterol checked during a routine health screening.
In Singapore, the Health Promotion Board (HPB) recommends that adults aged 40 and above go for regular health screenings, including cholesterol checks, at least once every three years. However, younger adults with risk factors such as obesity, diabetes, or a family history of heart disease should also consider early screening.
Peripheral Arterial Disease: A Clue in Your Toenails
Despite its silent nature, high cholesterol can sometimes manifest through subtle physical changes. One such indicator is peripheral arterial disease (PAD), a condition where fatty deposits build up in the arteries, particularly those supplying the legs. PAD is a common yet underdiagnosed condition, especially in older adults and those with risk factors such as diabetes, smoking, or a family history of cardiovascular disease.
According to the NHS, PAD can cause "brittle, slow-growing toenails." This occurs because reduced blood flow deprives the toenails of essential nutrients and oxygen, leading to changes in their appearance and growth rate. Other warning signs in the feet include:
- Hair loss on the legs and feet
- Ulcers or sores on the feet that are slow to heal
- Coldness or numbness in the lower legs or feet
- Weak or absent pulse in the legs or feet
- Shiny skin on the legs
A common symptom of PAD is a painful ache in the legs whilst walking, known as claudication, which typically eases after a few minutes of rest. Both legs are usually affected, though one may be worse than the other. These symptoms often develop gradually, making them easy to overlook.
In Singapore, a study published in the Annals, Academy of Medicine, Singapore found that PAD affects about 3% to 10% of the general population, with prevalence increasing with age and amongst those with diabetes or hypertension.
Why Early Detection Matters
PAD is not just a problem for your legs—it is a red flag for your overall cardiovascular health. People with PAD are at significantly higher risk of heart attacks, strokes, and other complications. Early detection of these subtle symptoms, such as changes in your toenails, can prompt timely medical intervention and potentially prevent more serious health issues.
Who Is at Risk?
Several factors can increase your risk of developing high cholesterol and PAD, including:
- Age (risk increases with age)
- Family history of heart disease or high cholesterol
- Smoking
- Diabetes or high blood pressure
- Obesity or being overweight
- Sedentary lifestyle
- Unhealthy diet, particularly one high in saturated fats and trans fats
In Singapore, the National Population Health Survey 2022 reported that 8.9% of adults aged 18 to 69 are obese, and 8.5% have diabetes—both of which are significant risk factors for high cholesterol and PAD.
What Should You Do?
If you notice your toenails becoming brittle or growing more slowly than usual, or if you experience leg pain whilst walking, do not ignore these signs. Consult your GP or healthcare provider for a thorough assessment. A simple blood test can check your cholesterol levels, and further tests such as an ankle-brachial index (ABI) can help diagnose PAD.
The good news is that high cholesterol and PAD are both manageable and, in many cases, preventable. The NHS, HPB, and health experts recommend the following steps:
- Adopt a heart-healthy diet: Focus on fruits, vegetables, whole grains, lean proteins, and healthy fats such as those found in olive oil, nuts, and fish. Limit saturated fats, trans fats, and processed foods.
- Exercise regularly: Aim for at least 150 minutes of moderate-intensity aerobic activity each week, such as brisk walking, cycling, or swimming.
- Maintain a healthy weight: Losing excess weight can help lower cholesterol and reduce your risk of cardiovascular disease.
- Quit smoking: Smoking damages blood vessels and accelerates the build-up of fatty deposits in the arteries.
- Limit alcohol consumption: Excessive drinking can raise cholesterol levels and blood pressure.
- Take prescribed medication: If lifestyle changes are not enough, your doctor may prescribe statins or other cholesterol-lowering medications.
Whilst high cholesterol often goes unnoticed, paying attention to small changes—like the condition of your toenails—could provide an early warning of underlying cardiovascular issues. Early action, including regular health screenings and lifestyle adjustments, can make all the difference to your long-term health and well-being.
If you have any concerns about your cholesterol or notice unusual changes in your feet or legs, seek medical advice promptly. Prevention and early intervention remain the best strategies for protecting your heart and overall health.
If You’ve Noticed Nail Changes: A Calm, Step-by-Step Check (What Matters Most)
Nail changes can be a useful prompt to look after your cardiovascular health — but they are common and often have non-cardiac causes. The point is to use the clue wisely: check circulation risk, then confirm with proper tests.
1) First: rule out common non-cholesterol causes
- Footwear friction / trauma: tight shoes and repeated pressure can make nails brittle or ridged.
- Fungal infection: thickened, discoloured, crumbly nails are often fungal rather than vascular.
- Skin conditions: eczema/psoriasis can affect nails.
- Nutritional factors: low iron or poor overall nutrition can contribute to brittle nails.
2) Then: check for circulation red flags (PAD clues)
Nail changes matter more when they come with any of the following:
- Leg pain/cramp when walking that eases with rest
- Cold feet or one foot colder than the other
- Slow-healing cuts/ulcers on toes/feet
- Hair loss on lower legs, shiny skin, or colour changes
- Numbness or reduced sensation (especially in diabetes)
3) What to ask for at a clinic (simple, practical script)
- “Can we check my blood pressure and review my cardiovascular risk?”
- “Can I do a lipid profile (LDL, HDL, triglycerides) and a glucose/HbA1c test?”
- “Can you check pulses in my feet — and do I need an ankle–brachial index (ABI) test for circulation?”
- “If this is not circulation-related, should I treat for fungal infection or see a podiatrist/dermatologist?”
4) What to do whilst you’re waiting for tests
- Move daily: gentle walking supports circulation (stop and seek advice if pain is severe).
- Foot care basics: keep feet clean/dry; moisturise skin (not between toes); trim nails carefully.
- If you smoke, prioritise quitting: it’s one of the biggest PAD risk multipliers.
- Upgrade the plate: more fibre, less deep-fried/ultra-processed foods; choose unsaturated fats more often.
Medical note: Seek urgent care if you develop sudden severe leg pain, a cold/pale foot, rapidly worsening wounds, or sudden loss of sensation. This article is for general education and is not a substitute for medical advice.
Editorial update: 22 February 2026 — expanded with a “nails are a clue, not a diagnosis” clarification, a PAD red-flag checklist, and a clinic question script.
Note: This piece was written as a commissioned feature and has appeared in other health and lifestyle platforms.